Dinges, D. F., Whitehouse, W. G., Orne, E. C., Bloom, P. B., Carlin, M. M., Bauer, N. K., Gillen, K. A., Shapiro, B.S., Ohene-Frempong, K., Dampier, C., & Orne, M. T. Self-hypnosis training as an adjunctive treatment in the management of pain associated with sickle-cell disease. International Journal of Clinical and Experimental Hypnosis, 1997, 45, 417-432.
University of Pennsylvania School of Medicine, Philadelphia
The Children's Hospital of Philadelphia, Philadelphia, Pennsylvania
St. Christopher's Hospital for Children, Philadelphia, Pennsylvania
University of Pennsylvania School of Medicine, Philadelphia
Abstract: A cohort of patients with sickle cell disease, consisting of
children, adolescents, and adults, who reported experiencing three or more episodes
of vaso-occlusive pain the preceding year, were enrolled in a prospective two-period
treatment protocol. Following a 4-month conventional treatment baseline phase,
a supplemental cognitive-behavioral pain management program that centered on
self-hypnosis was implemented over the next 18 months. Frequency of self-hypnosis
group
Manuscript submitted July 29,1996; final revision received June 3,1997.
1 This research was performed at the Unit for Experimental Psychiatry, which, during the study, was located at the Institute of Pennsylvania Hospital. We gratefully acknowledge the research support provided by each of the following agencies: Grant MH44193 from the National Institute of Mental Health; the van Amerigen Foundation; Hasbro Foundation; MBNA America Bank, N.A.; Stratford Foundation; Arcadia Foundation; Curry Foundation; the Auxiliary of Pennsylvania Hospital; the Commonwealth of Pennsylvania; and the Institute for Experimental Psychiatry Research Foundation.
2 Several colleagues provided invaluable assistance and advice in the development of the research and treatment protocols, including David Barlow, Ph.D., Jean Chapman, Ph.D., Campbell W. Perry, Ph.D., Karl Rickels, M.D., and Howard Roffwarg, M.D. Finally, we are indebted to the following individuals for their professional and technical contributions to the study: Brad L. Bates, Ph.D., John Durocher, M.D., Roy Gay, M.D., Barbara Haupt, R.N., Robert Nadon, Ph.D., Geoffrey Ott, Darcy Reber, Linnette B. Reilly, RN., Kim Steinberg, and Angela Tuohey.
3 Requests for reprints should be addressed to David F. Dinges, Ph.D., Unit for Experimental Psychiatry, University of Pennsylvania School of Medicine, 1013 Blockley Hall, 423 Guardian Drive, Philadelphia, PA 19104-6021.
417
418 DAVID F. DINGES ET AL.
training sessions began at once per week for the first 6 months, became biweekly for the next 6 months, and finally occurred once every third week for the remaining 6 months. Results indicate that the self-hypnosis intervention was associated with a significant reduction in pain days. Both the proportion of "bad sleep" nights and the use of pain medications also decreased significantly during the self-hypnosis treatment phase. However, participants continued to report disturbed sleep and to require medications on those days during which they did experience pain. Findings further suggest that the overall reduction in pain frequency was due to the elimination of less severe episodes of pain. Non- specific factors may have contributed to the efficacy of treatment. Nevertheless, the program clearly demonstrates that an adjunctive behavioral treatment for sickle cell pain, involving patient self-management and regular contact with a medical self-hypnosis team, can be beneficial in reducing recurrent, unpredictable episodes of pain in a patient population for whom few safe, cost-effective medical alternatives exist.
Sickle cell disease (SCD) is a genetic disorder that afflicts primarily persons of African heritage and is characterized by periodic deformation (i.e., "sickling") of red blood cells. The sickle-shaped cells occlude blood vessels and capillaries, promoting unpredictable episodes of ischemic pain, organ failure, and other serious health problems, in addition to being associated with a shortened lifespan (Gil, 1989; Nagel, Fabry, Billett, & Kaul, 1987; Segal, 1989). It is estimated that 1 out of every 300 to 400 African American newborns is afflicted with some form of sickle hemoglobinopathy; approximately 25% to 35% of these have a milder form of the disease (i.e., SC hemoglobinopathy or sickle beta-thalassemia), whereas approximately 65% to 75% suffer from the more severe variant -- sickle cell anemia (i.e., SS hemoglobinopathy) (Ranney, 1992).
There are, as yet, no specific medical treatments for SCD. Those treatments that have been employed are usually directed at the most salient symptom of SCD -- the intermittent episodes of pain produced by vaso-occlusion, which can last from a few hours to several weeks (Gil, 1989; Shapiro, 1993). Mild to moderate pain episodes are typically managed at home with nonnarcotic analgesics; more severe crises may require emergency room treatment, often consisting of hydration and narcotics, with occasional blood transfusions for cases involving other serious medical complications (Shapiro, 1989, 1993). Although there have been some promising results using hydroxyurea therapy to decrease the concentration of hemoglobin susceptible to sickling (Charache et al., 1992; Eaton & Hofrichter, 1995; Scott, Hillery, Brown, Misiewicz, & Labotka, 1996), these findings are preliminary and do not obviate the need for management of pain when it does occur.
Estimates based on medical records from sickle cell clinics, emergency rooms, and hospitals indicate that 10% to 20% of patients with SCD have frequent pain, 40% to 50% have some pain, and 30% to 40% have no pain (Platt et al., 1991; Vichinsky, Johnson, & Lubin, 1982). However, in a pro-
419 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
spective study using daily diaries in a cohort of patients with high rates of sickle cell pain followed from 10 to 24 months, we found that 89% of SCD pain episodes did not involve hospitalization (Shapiro, Dinges, Orne, Ohene-Frempong, & Orne, 1990). Thus, reliance on hospitalization records may seriously underestimate the incidence of SCD pain among a population that is often disadvantaged socioeconomically, medically underserved, and at times poorly treated by the health care system due to disbelief in the severity of their pain or their need for narcotics, especially during emergency room visits (Payne, 1989; Shapiro, 1993).
Equally important is consideration of the impact of these "silent" pain episodes on work productivity and school attendance. Some studies have found that children who experience SCD pain do not appear to be psychosocially disadvantaged relative to ethnically and socioeconomically matched controls (Kumar, Powers, Allen, & Haywood, 1976; Lemanek, Moore, Gresham, Williamson, & Kelley, 1986). However, our preliminary work suggests that children and adolescents with frequent SCD pain may be behaviorally disadvantaged in that they restrict their activities and are absent from school on 30% of the days they have pain (Shapiro et al., 1995). We have shown that they also have disturbed sleep from the pain and are at risk for development of a significant sleep debt that can exacerbate problems with daytime functioning and school attendance (Dinges et al., 1990).
Patients with SCD who have frequent and severe pain usually have this problem throughout their lives, and the extent of pain progresses with age (Platt et al., 1991). If they are to be productive and independent, they must learn to cope with and control their pain in such a way that the pain itself, as well as the methods for its control, interferes as little as possible with their everyday activities and quality of life. Given the paucity of effective medical treatments, coupled with the unpredictability of pain onset and the side effects of narcotic therapy, such patients are prime candidates for training in cognitive-behavioral interventions for pain management (Turk, Meichenbaum, & Genest, 1983; Vichinsky et al., 1982). Relevant preliminary studies and case reports have used biofeedback modalities (Cozzi & Tryon, 1987; Thomas, Koshy, Patterson, Dorn, & Thomas, 1984), relaxation (Thomas, Talischy, & Washington, 1984), and hypnosis (Zeltzer, Dash, & Holland, 1979), with encouraging results.
Guided by the substantial evidence for hypnotic analgesia (Orne & Dinges, 1989) in controlling experimentally induced pain (Meier, Klucken, Soyka, & Bromm, 1993; Miller & Bowers, 1993; Zeltzer, Fanurik, & LeBaron, 1989) or pain associated with medical/surgical procedures (Hilgard & LeBaron, 1984; Syrjala, Cummings, & Donaldson, 1992) and burn debridements (Patterson, Everett, Burns, & Marvin, 1992), we sought to design, implement, and evaluate a behavioral treatment program centered on self-hypnosis for SCD pain management at home. We report here find-
420 DAVID F. DINGES ET AL.
ings from the initial cohort of a larger two-period prospective investigation, featuring a 4-month conventional treatment (baseline) phase, followed by 18 months of conventional treatment combined with adjunctive self-hypnosis training.4
METHOD
Participants
Research participants were recruited from the sickle cell treatment clinics of area hospitals, following referral by one of the medical staff. This population represents primarily those individuals with high rates of severe pain that cannot be managed entirely at home (cf. Platt et al., 1991). Some patients who were eligible for participation declined due to religious beliefs pertaining to the practice of hypnosis. Volunteers who comprised the current study sample consisted of 37 individuals, 24 of whom had the homozygous sickle genotype (SS sickle cell anemia) and 12 of whom had a compound heterozygous hemoglobin genotype (SC disease); 1 individual had sickle SB0-thalassemia. Criteria for inclusion in the study required being between 5 and 60 years of age, retrospectively reporting at least three vasa-occlusive pain episodes that were not treated by blood transfusion during the year prior to enrollment, and identification of SCD pain as a significant problem. Eleven participants (5 male; 6 female) ranged in age from 5 to 11 years; 17 participants (7 male; 10 female) were between 12 and 19 years of age; and 9 participants (4 male; 5 female) were between 20 and 51 years of age.
Procedure
Patients were referred by their primary care physicians, and in most cases, the enrollment sessions were conducted at the sickle cell clinics. The research protocol was approved by the Institutional Review Boards of the university and participating hospitals, and informed consent was obtained from all patients and their guardians by the first author. Following enrollment in the study, participants were instructed in the use of daily pain diaries (completed on awakening in the morning and again before bed), which provided key dependent variables regarding pain, medication, school/work attendance, sleep, and (following the baseline phase) practice of the behavioral self-hypnosis exercise (Shapiro et al., 1990). In the case of preadolescent participants, caregivers were taught, when necessary, how to help their children to complete the daily diaries. Because the study was designed to compare conventional treatment for SCD pain to conventional plus self-hypnosis treatment, patients were encouraged to continue to follow the medical treatment plan of their
4 Although a case-controlled study will ultimately be necessary to establish the efficacy of behaviorally based interventions for sickle cell disease pain, for a variety of reasons, including the acute need for treatment in this severely afflicted cohort, a two-period prospective design was adopted at this preliminary stage of investigation.
421 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
primary care physicians. This included taking their prescribed medications for pain (e.g., acetaminophen, NSAIDS, opioids) throughout the study and recording them in the diary. Regular telephone contact with the participants helped to ensure the timely receipt of completed diaries, which were returned to the research laboratory on a weekly basis using procedures detailed elsewhere (Shapiro et al., 1990).
Behavioral treatment sessions, which included training in self-hypnosis (Soskis, 1986), were held at the laboratory weekly for the first 6 months, then biweekly for 6 months, then once every 3 weeks for 6 months. The sessions were conducted in small (n = 6 to 12), age-appropriate groups by one or both of two senior psychiatrists with extensive experience in the use of hypnosis for pain control. Family and friends of the patients, especially primary caregivers of the children, were invited to participate in the training sessions, and a number of them did so on a frequent basis. The general content of these sessions consisted of an opportunity to practice self-hypnosis, ideomotor exercises that most participants could successfully master (e.g., hands moving together, arm becoming lighter and rising, etc.), group discussion of participants' subjective experiences, encouragement, and efforts to develop effective therapeutic metaphors and self-suggestions for pain management.5 There was no purposive attempt to assess hypnotizability due to (a) the wide age range of the sample, which precluded the use of any single standardized instrument for all participants; (b) the program objectives, which sought to identify cost-effective group, rather than individualized, intervention strategies; and (c) concerns that poor performance on a formal test of hypnotic susceptibility might undermine motivation as well as commitment to the self-hypnosis training program (cf. Orne, Whitehouse, Dinges, & Orne, 1996).6
5 Specific details of the therapeutic procedures and objectives can be obtained from the manuscript titled "Treatment Manual: Self-Hypnosis Training Groups for the Management of Vaso-Occlusive Crisis Pain in Sickle Cell Disease," © Unit for Experimental Psychiatry, 1989-1992, which has been deposited with the National Auxiliary Publications Service (NAPS). For 43 pages, order Document No 05419 from NAPS, c/o Microfiche Publications, P. O. Box 3513, Grand Central Station, New York, NY 10163-3513. Remit in advance, in U.S. funds only, $14.95 for photocopies or $5.00 for microfiche, and make checks payable to Microfiche Publications-NAPS. There is a $15.00 invoicing charge on all orders filled before payment. Outside the United States and Canada, add postage of $6.50 for a photocopy and $1.75 for a fiche.
6 As an exercise intended to familiarize patients with a varied range of hypnotic experiences, the Harvard Group Scale of Hypnotic Susceptibility, Form A (HGSHS:A; Shor & Orne, 1962) was administered to 29 of the 40 study participants (HGSHS:A M = 6.14, SD = 2.23) near the midpoint of the investigation. There were no significant correlations between this index of hypnotizability and any of the baseline or outcome measures of the study, nor were there any reliable age-group differences in HGSHS:A scores. However, the HGSHS:A may not be an appropriate measure of hypnotic ability for younger participants, as norms are unavailable for persons under 18 years of age. Moreover, in the present sample, there were substantial discrepancies (i.e., greater than 40%) between self-reported HGSHS:A scores and those provided by experienced observers, who judged the participants to be asleep during a number of the scale items.
422 DAVID F. DINGES ET AL.
RESULTS
Daily Diary Compliance and Validity
Throughout both baseline and treatment periods of the current study, participants completed a total of 21,237 daily pain diaries (84% compliance). The diary compliance rate during the conventional treatment baseline phase was comparable to that during the behavioral + conventional treatment phase (87% and 83%, respectively).
To ascertain the validity of the pain diary data, two lines of epidemiological evidence were relied on. First, incidence and severity of SCD pain has been found to be positively associated with age (Platt et al., 1991). In the current sample, Kruskal-Wallis tests determined that both the percentage of baseline days with SCD pain, H(2) = 7.47, p = .024, and the mean SCD pain intensity rating during baseline, H(2) = 7.27, p = .026, varied as a function of age group, with children (age 5-11) reporting fewer SCD pain days, U(11,12) = 26.0, p = .014, and less intense pain, U(11,12) = 23.0, p = .008, than adults (age 20-51); adolescents reported intermediate values on these two measures. A second approach toward validating the diary data was to investigate whether the type of sickle hemoglobinopathy (SS vs. SC) affected the severity of SCD pain (cf. Platt et al., 1991). Analyses of baseline diary records revealed that participants with sickle cell anemia (SS genotype) had significantly longer duration pain episodes than participants with the less severe sickle SC disease, SS M = 4.4 days, SC M = 2.2 days; U(12,24) = 84.5, p = .046. The general correspondence between these baseline data and epidemiological reports in the literature provides support for the validity of the pain reports obtained with the daily diary system.
Impact of the Behavioral/Self-Hypnosis Treatment Relative to Baseline
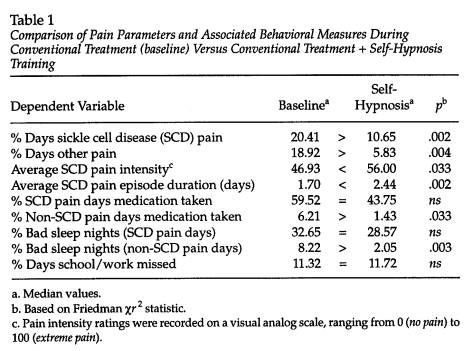
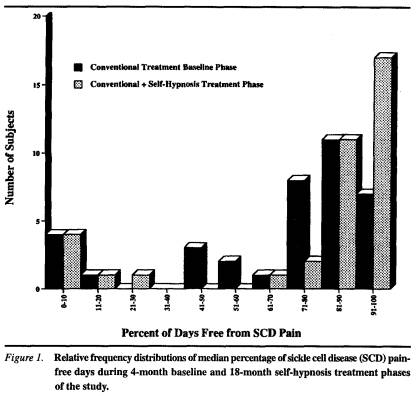
Changes from baseline to behavioral treatment periods in SCD pain parameters and pain-related biobehavioral measures were evaluated using Friedman's analysis of variance by ranks. Median values and two-tailed significance levels for the relevant comparisons are provided in Table 1. These analyses revealed that vaso-occlusive pain frequency (percentage of days with SCD pain) was significantly diminished following the introduction of the self-hypnosis treatment component, Xr2(1) = 9.76, p = .002. This reduction in reported SCD pain proportions is clearly evident in the relative frequency distributions of pain-free days portrayed in Figure 1. Training in self-hypnosis appears to have shifted a number of participants with baseline rates of pain-free days in the 41%-80% range to above the 90% level. The only measure that distinguished patients who achieved this optimal decrease in SCD pain frequency was a significant reduction from baseline to self-hypnosis phases in reliance on pain medication, Xr2(1) = 7.36, p = .007; patients who experienced more modest levels of improvement were less likely to
423 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN

reduce their use of medications for pain management, Xr2(l) = 0.17, p > .10. In fact, 9 participants (24%) failed to show any reduction in SCD pain frequency during the behavioral treatment phase. These refractory patients differed from the 28 others (76%) only in terms of relying more on medication to manage SCD pain at baseline, U(l) = 186.00, p = .034. In addition to reducing the frequency of SCD pain, however, self-hypnosis training was also associated with a reliable decrease in reports of "other" pain, Xr2(l) = 8.53, p = .004, relative to the conventional treatment baseline phase (Table 1).
Although SCD pain frequency decreased during the behavioral treatment period, Table 1 indicates that the median average intensity of SCD pain was greater relative to baseline, Xr2(1) = 4.57, p = .033, as was the average duration of SCD episodes, Xr2(l ) = 9.76, p = .002. This suggests that the behavioral self-hypnosis treatment program helped to eliminate milder episodes of vaso-occlusive pain, but it was not as effective against the more severe occurrences of SCD pain.
The overall effects of the self-hypnosis intervention on pain medication use varied depending on whether patients were experiencing episodes of SCD pain or not. Thus, as Table 1 shows, there was no significant reduction in the percentage of SCD pain days that required medication, Xr2 (1) = 1.73, p > .10. This was expected given that patients were urged to follow their physicians' instructions to continue to use their medication for severe pain episodes. However, the tendency to take such medications on other than SCD pain days, which was already comparatively
424 DAVID F. DINGES ET AL.
low at 6% of baseline days (vs. 60% of baseline SCD pain days; Xr2(l) = 21.19, p < .001), was reduced to 1% of days during the self-hypnosis treatment phase, Xr2(l) = 4.57, p = .033.
A similar dependency on the presence versus absence of SCD pain episodes was found to modulate the impact of self-hypnosis training on nighttime sleep quality. As indicated in Table 1, self-hypnosis training was associated with a significant reduction in the percentage of bad sleep nights, but only for days when patients were not experiencing an SCD pain episode, Xr2(l) = 8.76, p = .003; during episodes, there was no reliable change from baseline in the percentage of bad sleep nights, Xr2(l) = 0.68, p > .10. As is evident from Table 1, during both baseline and self-hypnosis treatment phases, there was proportionately more bad sleep associated with SCD pain than there was on nights with no SCD pain.
The median percentage of days during which school or work was missed was 11% at baseline, but there were consistently large individual differences in absenteeism at both baseline and treatment phases (range: 0% -51%). Thus, as indicated in Table 1, self-hypnosis training had no apparent effect on absenteeism from school or work, Xr2(l) = 2.46, p > .10.
425 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
Effects of Frequency of Self-Hypnosis Training Sessions and Individual Practice
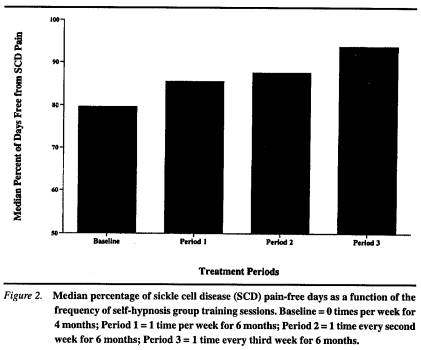
In an effort to determine whether the frequency at which self-hypnosis training sessions were conducted influenced treatment gains, the proportion of days free from SCD pain was analyzed over the 4 months of baseline and 18 months of treatment, which included consecutive 6-month periods during which sessions occurred weekly, then biweekly, and finally, once every 3 weeks. On average, patients attended 74% of the training sessions. The most common reason for missing a session was illness or hospitalization. As depicted in Figure 2, there was a monotonic increase across phases in the percent of pain-free days, Xr2(3) = 7.34, p = .06. Follow-up analyses indicated that the percentage of pain-free days increased significantly from baseline to Treatment Period 1, Xr2(l) = 9.76, p = .002. Results from Period 2 were not significantly different from either Period 1, Xr2(l) = 0.03, p > .10, or baseline, Xr2(l) = 2.13, p > .10; Period 3 results were above baseline, Xr2(l) = 5.40, p = .02. Although the percentage of pain-free days increased across study phases, the effect was not related to rates of self-hypnosis practice outside the group training sessions (r = 0.09, p = .64). Similarly, the rate of self-hypnosis practice did not vary among the three age groups, F(2, 29) = 1.66, p = .21.
426 DAVID F. DINGES ET AL.
DISCUSSION
The findings of the current study indicate that a cognitive-behavioral program, featuring self-hypnosis training, can be effectively integrated into a conventional medical treatment approach to the management of recurrent, unpredictable episodes of vaso-occlusive pain associated with SCD. Moreover, such a program appears to be efficacious, reducing the frequency of SCD pain episodes, as well as non-SCD pain. This suggests that, among other possibilities, participants were able to generalize the cognitive-behavioral intervention to types of pain other than those which they attribute to SCD.
It is noteworthy that, although the proportion of pain days decreased during the self-hypnosis treatment phase, neither the intensity nor duration of SCD pain episodes was reduced. In fact, vaso-occlusive pain episodes were rated as more intense relative to baseline and had a mean duration that was 1 1/2 days longer during the behavioral self-hypnosis treatment phase. We believe this is a direct result of the intervention's capacity to eliminate a substantial proportion of mildly to moderately painful episodes, leaving the more severe episodes (in intensity of pain and with longer duration). That is, there was less pain overall during the self-hypnosis treatment phase, but that which did occur tended to be the more severe episodes. Such a finding is consistent with expectations that a behavioral intervention should be better suited to alleviating less severe rather than more severe bouts of pain.
A related pattern of findings was observed for the impact of the treatment program on the number of days that pain medication was taken. Although patients were not told to reduce their medication intake during the self-hypnosis treatment phase, many of them had this as a motivating factor when joining the program. Accordingly, patients decreased to one third the proportion of days overall (i.e., pain + pain-free days) that they used pain medication. Nevertheless, when more severe SCD pain was experienced, pain medication was not less likely to be used. Apart from indicating that patients still need medications to manage SCD pain, this observation suggests that participants' diary reports of medication usage are reliable. If patients were falsely reporting less medication use to comply with demand characteristics of the self-hypnosis intervention, then one would also expect to find a significant reduction in medications on SCD pain days. This was not the case.
The use of pain medication also provided insight into the failure of the treatment program to reduce the proportion of SCD pain days in some patients. Among the 37 participants treated in the study, 28 had a decrease in the proportion of SCD pain days from baseline to treatment, whereas 9 participants did not. Of the various pain parameters assessed, the single variable that significantly discriminated between treatment responders and nonresponders was the use of pain medication. Those participants who were able to reduce their proportion of pain days used
427 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
significantly less pain medication on SCD pain days at baseline -- before the self-hypnosis intervention. It remains to be determined what mediates the relationship between frequency of pain medication use and degree of benefit from cognitive-behavioral approaches to pain management. An additional limitation of the current study is that the sample size was too small to have reliably identified many other factors that may have contributed to the therapeutic efficacy of the program (e.g., illness behavior, family involvement, pain coping strategies). Nevertheless, the finding that use of pain medication was the singular discriminative variable between those who benefited from self-hypnosis and those who did not suggests that, as an adjunct to the medical management of pain, a trial of behavioral intervention involving self-hypnosis focused on pain management may be a prudent therapeutic strategy for any individuals with high rates of SCD pain.
Many participants spontaneously reported that pain disturbed their sleep, and the data in Table 1 confirm this. The proportion of nights rated as "bad" sleep was significantly reduced during the treatment phase, relative to baseline, but the effect was evident only on pain-free days and not on SCD pain days. This effect probably reflects an emphasis in the treatment protocol on good sleep hygiene to foster overall well-being. Indeed, during the group self-hypnosis training sessions, a number of participants pointed out that they had made modifications to their bedtime routines, including practicing their self-hypnosis exercise, as a way of promoting sleep. Thus, the treatment phase was associated with fewer poor nights of sleep when no pain was experienced, but when SCD pain occurred, not surprisingly, sleep hygiene could not prevent sleep disturbance.
Although the cognitive-behavioral intervention reduced the proportion of days that SCD pain was experienced and pain medication was taken, it had no statistically reliable effect on school and work attendance. It should be noted that, in this study, most of the absenteeism was found among children and adolescents, relative to school attendance -- adults rarely were absent from work, until they were too disabled to work at all. In an earlier study of 18 children and adolescents followed for a total of 3,186 school days (Shapiro et al., 1995), we observed that approximately half of all absences from school were on days that participants experienced SCD pain. Clearly, SCD adversely affects school attendance. However, the same study identified the presence of relatively stable individual differences in school absenteeism, encompassing both SCD pain days and days without pain. Thus, school attendance appears to be multifactorially determined. As such, it is less likely to be influenced by behavioral interventions directed at pain management than are pain outcomes per se.
The current investigation also assessed the importance of frequency of group self-hypnosis training sessions in promoting reductions in the
428 DAVID F. DINGFS ET AL.
number of SCD pain episodes. That is, group sessions were scheduled every week for the first 6 months, then were conducted biweekly for 6 months, and finally, once every 3 weeks for 6 months. It would appear that weekly sessions with patients early in treatment yielded the greatest gains, although the order of training intensity periods was not counterbalanced to assess frequency of sessions independent of order or time-in-study. Nevertheless, there continued to be reductions in SCD pain proportions more than 1 year later, when patients were being seen only once every 3 weeks. This suggests that, following adequate early training, the benefits of the treatment program persist with occasional "booster" group sessions. The extent to which treatment gains can be maintained with such minimal contact is an important consideration in determining the cost-effectiveness of the behavioral intervention.
It is not clear what the salient factors were in producing the beneficial effects of the treatment package when used in conjunction with conventional medical treatment for SCD pain. This inherent limitation of the study derives from the small sample size, which precluded an exhaustive analysis of the various factors associated with pain reduction. There was, however, no evidence that the rate at which patients practiced self-hypnosis at home related to the magnitude of the treatment effect. Nevertheless, most patients (76%) benefited during the self-hypnosis treatment phase. This suggests that the intervention, with its emphasis on learning to control pain, served to empower patients to manage their pain more actively and effectively. It is noteworthy that patients unanimously expressed a desire to continue the training sessions at the end of the study and that they requested, and were provided with, an audiotape of the medical coach's self-hypnosis sample exercise.7
Beyond self-hypnosis training per se, the intervention involved a number of factors that also may have contributed to pain reduction. These nonhypnotic factors included (a) patients' high motivation to control their pain and reduce the need for medications; (b) family and peer-based group social support; (c) patients' perceptions of a therapeutic relationship with a caring medical professional team; and (d) reduction of patients' anxiety through appropriate education about SCD and pain. These factors, combined with the heterogeneity of the limited patient sample size (i.e., range of ages, pain rates, and sickle hemoglobinopathies) likely prevented the observation of any specific relationship among a participant characteristic, treatment component, and outcome. This lack of specificity of the treatment process notwithstanding, the study does demonstrate that a medically underserved patient cohort, with severe and frequent organically based pain, can be helped by an adjunctive cognitive-behavioral treatment program structured in a socially supportive and caring milieu.
7 This demonstration self-hypnosis training program was supported as a research protocol, which was limited in time by research funding.
429 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
REFERENCES
Charache, S.., Dover, G. J., Moore, R D., Eckert, S., Ballas, S. K., Koshy, M., Milner, P., Orringer, E. P., Phillips, G., Jr., Platt, O. S., & Thomas, G. H. (1992). Hydroxyurea: Effects on hemoglobin F production in patients with sickle cell anemia. Blood, 79, 2555-2565.
Cozzi L., & Tryon, W. W. (1987). The effectiveness of biofeedback-assisted relaxation in modifying sickle cell crises. Biofeedback and Self-Regulation, 12, 51-61.
Dinges, D. F., Shapiro, B.S., Reilly, L. B., Orne, E. C., Ohene-Frempong, K., & Orne, M. T. (1990). Sleep/wake dysfunction in children with sickle cell crisis pain. Sleep Research, 19, 323.
Eaton, W. A., & Hofrichter, J. (1995). The biophysics of sickle cell hydroxyurea therapy. Science, 268, 1142-1143.
Gil, K. M. (1989). Coping with sickle cell disease. Annals of Behavioral Medicine, 11, 49-57.
Hilgard, J. R, & LeBaron, S. (1984). Hypnotherapy of pain in children with cancer. Los Altos, CA: William Kaufmann.
Kumar, A., Powers, D., Allen, J., & Haywood, L. J. (1976). Anxiety, self-concept, and personal and social adjustments in children with sickle cell anemia. Journal of Pediatrics, 88, 859-863.
Lemanek, K. L., Moore, S. L., Gresham, F. M., Williamson, D. A., & Kelley, M. L. (1986). Psychological adjustment of children with sickle cell anemia. Journal of Pediatric Psychology, 11, 397-410.
Meier, W., Klucken, M., Soyka, D., & Bromm, B. (1993). Hypnotic hypo- and hyperalgesia: Divergent effects on pain ratings and pain-related cerebral potentials. Pain, 53, 175-181.
Miller, M. E., & Bowers, K. S. (1993). Hypnotic analgesia: Dissociated experience or dissociated control? Journal of Abnormal Psychology, 102, 29-38.
Nagel, R L., Fabry; M. E., Billett, H. H., & Kaul, D. K. (1987). Sickle cell painful crisis: A multifactorial event. Progress in Clinical and Biological Research, 240, 361-380.
Orne, E. C., Whitehouse, W. G., Dinges, D. F., & Orne, M. T. (1996). Memory liabilities associated with hypnosis: Does low hypnotizability confer immunity? International Journal of Clinical and Experimental Hypnosis, 44, 354-369.
Orne, M. T., & Dinges, D. F. (1989). Hypnosis. In P. D. Wall & R Melzack (Eds.), Textbook of pain (2nd ed., pp. 1021-1031). London: Churchill Livingstone.
Patterson, D. R., Everett,J. J., Burns,G. L., & Marvin,J. A. (1992). Hypnosis for the treatment of burn pain. Journal of Consulting and Clinical Psychology, 60, 713-717.
Payne, R (1989). Pain management in sickle cell disease: Rationale and technique. Annals of the New York Academy of Sciences, 565, 189-206.
Platt, O. S., Thorington, B. D., Brambilla, D. J., Milner, P. F., Rosse, W. F., Vichinsky, E., & Kinney, T. R (1991). Pain in sickle cell disease: Rates and risk factors. New England Journal of Medicine, 325, 11-16
Ranney, H. M. (1992, January). The spectrum of sickle cell disease. Hospital Practice, pp.133-163.
Scott, J. P., Hillery, C. A., Brown, E. R., Misiewicz, V.,& Labotka, R J. (1996). Hydroxyurea therapy in children severely affected with sickle cell disease. Journal of Pediatrics, 128, 820-828.
Segal, M. (1989, March). New hope for children with sickle cell disease. FDA Consumer, pp. 14-19.
Shapiro, B. S. (1989). The management of pain in sickle cell disease. Pediatric Clinics of North America, 36, 1029-1045.
Shapiro, B. S. (1993). Management of painful episodes in sickle cell disease. In N. L. Schechter, C. B. Berde, & M. Y. Yaster (Eds.), Pain in infants, children, and adolescents (pp. 385-410). Baltimore, MD: Williams & Wilkins.
Shapiro, B.S., Dinges, D. F., Orne, E. C., Bauer, N. K., Reilly, L. B., Whitehouse, W. G., Ohene-Frempong, K., & Orne, M. T. (1995). Home management of sickle cell related
430 DAVID F. DINGES ET AL.
pain in children and adolescents: Natural history and impact on school attendance. Pain, 61, 139-144.
Shapiro, B. S., Dinges, D. F., Orne, E. C., Ohene-Frempong, K., & Orne, M. T. (1990). Recording of crisis pain in sickle cell disease. In D. Tyler & E. Krane (Eds.), Advances in pain research therapy (pp. 313-321). New York: Raven.
Shor R. E., & Orne, E. C. (1962). Harvard Group Scale of Hypnotic Susceptibility, Form A. Palo Alto, CA: Consulting Psychologists Press.
Soskis, D. A. (1986). Teaching self-hypnosis: An introductory guide for clinicians. New York: Norton.
Syrjala, K. L., Cummings, C., & Donaldson, G. W. (1992). Hypnosis or cognitive behavioral training for the reduction of pain and nausea during cancer treatment: A controlled clinical trial. Pain, 48, 137-146.
Thomas, J. E., Koshy, M., Patterson, L., Dorn, L., & Thomas, K. (1984). Management of pain in sickle cell disease using biofeedback therapy: A preliminary study. Biofeedback and Self-Regulation, 9, 413-420.
Thomas, J. E., Talischy, N., & Washington, A. (1984). Behavioral management of crisis in sickle cell disease and pain. Pain, 2, S99.
Turk, D. C., Meichenbaum, D., & Genest, M. (1983). Pain and behavioral medicine: A cognitive-behavioral perspective. New York: Guilford.
Vichinsky, E. P., Johnson, R, & Lubin, B. H. (1982). Multidisciplinary approach to pain management in sickle cell disease. American Journal of Pediatric Hematology/Oncology, 4, 328-332.
Zeltzer, L., Dash, J., & Holland, J. P. (1979). Hypnotically induced pain control in sickle cell anemia. Pediatrics, 64, 533-536.
Zeltzer, L., Fanurik., D., & LeBaron, S. (1989). The cold pressor pain paradigm in children: Feasibility of an intervention model (Part II). Pain, 37 , 305-313.
Zusammenfassung: Eine Kohorte von Patienten mit Sichelzellenanamie, die
aus Kindern, Volljahrigen, und Erwachsenen bestand, die berichteten drei oder
mehr Episoden vaso-okklusive Schmerzen im zuruckliegenden Jahr erfahren zu haben,
wurden in ein prospektives Behandlungsprotokol mit zwei Perioden einbezogen.
Nach einer vierwochigen konventionellen Behandlung als Baselinephase, wurde
ein zusatzliche kognitiv-verhaltenstherapeutische Schmerztherapie, die die Selbsthypnose
in den Mittelpunkt stellte, fur 18 Monate absolviert. Die Selbsthypnosesitzungen
fanden die ersten sechs Monate wochentlich statt, uber die nachsten sechs Monate
im zwei Wochen Rhythmus und schlieB lich fur die letzten sechs Monate alle drei
Wochen. Die Ergebnisse zeigen, daB die Selbsthypnose Behandlung mit einer signifikanten
Reduzierung derTage mil Schmerzen einhergehen. Sowohl das Verhaltnis der Nachte
mit schlechtem Schlaf, wie auch die Verwendung von Schmerzmitteln verringerte
sich wahrend des Selbsthypnose Behandlungsphase signifikant. Jedoch berichteten
die Teilnehmer der Studie, daB sie weiterhin an den Tagen, an denen sie Schmerzen
hatten, unter Schlafstorungen litten und Medikamente benotigten. Die Befunde
deuten weiterhin daraufhin, daB die Reduktion in der Haufigkeit der Schmerzen
durch die Unterdruckung von
431 SELF-HYPNOSIS FOR SICKLE CELL DISEASE PAIN
Episoden mit geringeren Schmerzen zustandekommt. Nichtsdestotrotz zeigt das Programm deutlich, daB eine zusatzliche Behandlung auf der Verhaltensebene bei Schmerzen derch Sichelzellenanamie, das Selbstmanagement beim Patienten und regelmaBigen Kontakt mit einem medizinischen Selbsthypnoseteam umfaBt, bei der Reduktion von wiederkehrenden, unvorhersehbaren Schmerzepisoden hilfreich sein kann, gerade in einer Patientenpopulation, fur die nur wenige kosteneffektive medizinische Altemativen existieren.
Resume: Une cohorte de patients souffrant d'anemie a globules rouges/faucille, composee d'enfants, d'adolescent, et d'adultes, rapportant ressentir trois episodes ou plus de douleur vasa-occlusive durant l'annee precedente, a ete recrutee dans un protocole prospectif compose de deux periodes de traitement. Apres une periode de quatre mois de traitement conventionnel servant de niveau de base, un programme supplementaire de gestion de la douleur, cognitif-behavioral, centre sur l'auto hypnose, a ete applique durant les 18 mois suivant. La frequence des sessions de groupe d'entrainement a l'auto hypnose fut d'une par semaine pour les premiers six mois, puis devint bi hebdomadaire pour les six mois suivants et enfin passa a une fois par trois semaines pour les derniers six mois. Les resultats montrent que l'intervention d'auto hypnose a ete associee a une reduction significative du nombre de jours avec douleur. La proportion de nuits de "mauvais sommeil" ainsi que l'utilisation de medications anti douleur ont, tous les deux, diminue de facon significative durant la phase de traitement par auto hypnose. Cependant, les patients ont continue de rapporter un sommeil agite et le besoin de prendre une medication lors des jours ou ils ressentaient de la douleur. Les resultats suggerent que la reduction globale de la frequence de la douleur est due a l'elimination des periodes de douleur moins grave. Des facteurs non specifiques ont pu contribuer a l'efficacite du traitement Quoiqu'il en soit, le programme demontre clairement que l'ajout d'un traitement behavioral pour l'anemie a globule rouge/faucille, traitement impliquant l'auto cantrole et un contact regulier avec une equipe medicale specialisee en auto hypnose, peut etre benefique par la reduction d'episodes recurrents et imprevisibles de douleur, chez une population de patients pour qui peu d'interventions medicales securitaires et effectives en termes de cout/efficacite existent
432 DAVID F. DINGES ET AL.
Resumen: Un conjunto de pacientes que padecia anemia de celulas falsiformes (SCD), conformado por ninos, adolescentes, y adultos, que reportaron haber sufrido tres o mas episodios de dolor vaso-oclusivo en el ano precedente, fueron enrolados en un protocolo de dos periodos prospectivos de tratamiento. Luego de una fase de cuatro meses de tratamiento convencional tomada como linea de base, se implanto un programa suplementario de manejo del dolor de tipo cognitivo-conductual centrado en la autohipnosis y que duro los siguientes dieciocho meses. La frecuencia de las sesiones del grupo de entrenamiento en autohipnosis comenzo con una por semana durante los primeros seis meses, continuo con dos semanales en los siguientes seis meses y finalmente se realizo una sesion cada tres semanas en los restantes seis meses. Los resultados indicaron que la intervencion autohipnotica estuvo asociada con una reduccion significativa de los dias de dolor. Tanto la proporcion de noches "mal dormidas" asi como el uso de medicamentos analgesicos tambien decrecio significativamente durante la fase de tratamiento autohipnotico. Sin embargo, los participantes continuaron reportando perturbaciones en el sueno y demandaron medicacion en aquellos dias en los que sintieron dolor. Hallazgos posteriores sugieren que la reduccion total de la frecuencia del dolor fue debida a la eliminacion de episodios menos severos de dolor. Factores no especificos pueden haber contribuido a la eficacia del tratamiento. Sin embargo, el programa demostro claramente que un tratamiento conductual adjunto para la anemia de celulas falsiformes que incluya el manejo por parte del propio paciente y un contacto regular con un equipo medico especializado en autohipnosis, puede ser beneficioso en reducir la recurrencia y los episodios impredecibles de dolor, en una poblacion de pacientes para la que existen pocas alternatives medicas, si se considera la relacion costo-e
ficacia.
The preceding paper is a reproduction of the following
article (Dinges, D. F., Whitehouse, W. G., Orne, E. C., Bloom, P. B., Carlin,
M. M., Bauer, N. K., Gillen, K. A., Shapiro, B.S., Ohene-Frempong, K., Dampier,
C., & Orne, M. T. Self-hypnosis training as an adjunctive treatment in the
management of pain associated with sickle-cell disease. International Journal
of Clinical and Experimental Hypnosis, 1997, 45, 417-432). It is reproduced
here with the kind permission of the Editor-in-Chief of The International Journal
of Clinical and Experimental Hypnosis.